Testicular cancer
Testicular cancer is most frequent in young males. It is the most common tumor in men in the 15 – 35 age group. There are three age peaks where testicular cancer is most common:
- 15 – 35 years (the most common age group)
- 0 – 10 years
- > 60 years
96% of all testicular tumors are malignant. Most present with metastases already present, but despite this the prognosis is excellent. Even advanced and metastatic testicular cancers are often curable. Overall the cure rate is 80 - 90%. Most (95%) of testicular malignancies are germ cell tumours, which originate from germ cells, the majority of these are seminomas.
Risk factors
Most are idiopathic, but some known risk factors exist:
- Cryptorchidism
- Previous testicular cancer
- Positive family history
- Gonadal dysgenesis
- Klinefelter syndrome
- Down syndrome
Pathology
95% of testicular tumors originate from germ cells. The remaining 5% originate from the testicular stroma (which is derived from the sex cords), including Sertoli cells, Leydig cells or granulosa cells. The classification can be visualised like this:
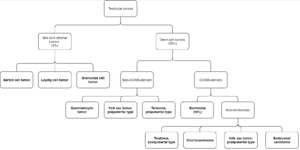
Germ cell tumours
Germ cell tumors develop from totipotent germ cells. During embryonal development these totipotent cells can travel down normal differentiation pathways and become spermatocytes. However, if they instead travel down abnormal developmental pathways, they can become seminomas or embryonal carcinomas. Embryonal carcinoma cells can then take one or more of these courses: They can undergo (intra)embryonic differentiation and form a (postpubertal) teratoma (which is comprised of embryonic tissues). They can undergo extraembryonic differentiation and form (postpubertal) yolk sac tumors or choriocarcinomas (which are extraembryonic tissues). Lastly the totipotent germ cells can remain undifferentiated and remain embryonal carcinoma. This is better illustrated on the figure below:

Germ cell tumors account for 95% of all testicular tumors. It’s very common (in 60% of cases) for germ cell tumors to contain more than one histological subtype. These are called mixed germ cell tumors. The remaining 40% of cases are pure germ cell tumors and contain only one histological subtype.
Most germ cell tumor develop from a precancerous lesion called germ cell neoplasia in situ (GCNIS). This precancerous lesion is virtually always present together with the mature GCNIS-derived germ cell tumor when examined histologically. This lesion has a 50% chance of progressing into cancer within 5 years.
Isochromosome 12p or extra copies of 12p is seen in almost all germ cell tumors.
GCNIS-derived germ cell tumours
Seminoma is the most common pure testicular germ cell tumor. It most frequently occurs in patients in their 40s. Seminomas grow slowly and rarely metastasize, and therefore have a better prognosis than non-seminomas. It also has a good radiosensitivity, meaning that it’s highly treatable by irradiation. Seminomas are homogenous masses with small foci of haemorrhage or necrosis. Some cases of seminoma can produce hCG.
Non-seminomas don’t respond as well to treatment as seminomas, and they metastasize earlier.
Embryonal carcinoma is most frequent in the 20 – 30-year age group. It frequently metastasizes. It’s most frequently found as a component of mixed germ cell tumors and is rarely found in pure form. The cells resemble primitive, embryonal cells and are therefore rapidly growing, often forming haemorrhage or necrosis.
Yolk sac tumor exists in two forms: the prepubertal type and the postpubertal type. In both forms the totipotent germ cells undergo extraembryonic differentiation and become yolk sac cells. Like the physiologic yolk sac, these tumors produce AFP (alpha-fetoprotein). The prepubertal form is the most common of the two. Structures resembling primitive glomeruli can be seen histologically, the so called Schiller-Duval bodies.
The postpubertal yolk sac tumor is a non-seminoma and is most frequently seen in adult mixed tumors. In the postpubertal type hemorrhage and necrosis is common.
Choriocarcinoma most frequently occurs in the 20 – 30-year age group. As the name implies, this tumor is formed when totipotent germ cells undergo extraembryonic differentiation and become placental cells. It’s the most aggressive type of testicular cancer, and therefore metastasizes very early and therefore often presents with symptoms of lung and brain metastases. Like the placenta this tumor produces hCG, so this tumor marker will be elevated. According to Dr. Bela this type also may contain foci of necrosis and hemorrhage.
Teratoma exists in two forms: the prepubertal type and the postpubertal type. In both forms the totipotent germ cells undergo (intra)embryonic (= somatic) differentiation and form somatic tissues from one or more germ layers. While teratomas are benign in females, they are malignant in males.
The postpubertal teratoma develops from GCNIS. It’s commonly found as a component of mixed germ cell tumors. It is malignant, unlike the prepubertal teratoma.
Mixed germ cell tumors account for 60% of all germ cell tumors, and as such most testicular tumours are mixed. They frequently produce AFP and/or hCG. These are the most frequent combinations:
- Embryonal carcinoma + seminoma
- Embryonal carcinoma + teratoma
- Embryonal carcinoma + teratoma + yolk sac tumor
Non-GCNIS-derived germ cell tumours
Spermatocytic tumor (also called spermatocytic seminoma) occurs most frequently in older men. It develops from spermatogonia, a post-pubertal germ cell, which explains why it only occurs in older men. It does not derive from GCNIS. It rarely metastasizes.
The prepubertal yolk sac tumor is the most common testicular tumor in children; the mean age upon diagnosis is 3 years old. This type is almost always pure. AFP is elevated.
The prepubertal teratoma is the second most common testicular tumor in children. Unlike most germ cell tumors it does not have isochromosome 12p. Contrary to the name it may also occur in adults, where it accounts for 20% of all teratomas. Prepubertal teratoma is benign, unlike the postpubertal type.
Sex cord stromal tumours
These tumors account for 5% of all testicular tumors in adults, but they are much more frequent in childhood. These tumors arise from Leydig cells, Sertoli cells or granulosa cells. They are usually benign.
Leydig cell tumors may produce testosterone, which can cause early puberty in children. Occasionally they can cause symptoms of femininization as well.
Lymphoma
Lymphomas may occur in the testes as well, most frequently as diffuse large B-cell lymphoma (DLBCL). These are the most frequent testicular tumors in men older than 60.
A summary of the different histological types of testicular cancer can be found in the table below.
| Tumor | Peak patient age | Tumor marker status | Important characteristic |
|---|---|---|---|
| Seminoma | Middle-aged adults (40 – 50) | 10% produce hCG | Good response to irradiation. Never necrotic. |
| Embryonal carcinoma | Young adults (20 – 30) | No tumor markers | Metastasize early. Necrotic and haemorrhagic tumor. |
| Choriocarcinoma | Young adults (20 – 30) | Produce hCG | Metastasize very early, most aggressive type |
| Mixed germ cell tumor | Young adults (15 – 30) | Produce hCG or AFP | Almost always includes embryonal carcinoma |
| Yolk sac tumor | Young children (< 5) | Produce AFP | Prepubertal type |
| Teratoma | All ages | No tumor markers | Benign if prepubertal type, malignant if postpubertal type |
| Spermatocytic tumor | Older adults (> 60) | No tumor markers | |
| Lymphoma | Older adults (> 60) | No tumor markers | Usually DLBCL |
Clinical features
Testicular tumors usually present as incidentally discovered firm, painless masses on the testis. Unlike hydroceles, these masses cannot be transilluminated. In case of metastases there may be symptoms like cough, chest pain, or bone pain.
Diagnosis and evaluation
The first diagnostic step for a testicular mass is ultrasound and physical examination. If these raise suspicion for malignancy, we proceed to orchidectomy.
Testicular masses are never biopsied, unlike most suspected tumors elsewhere in the body. Instead, sperm is cryopreserved, and the testis is removed by orchiectomy. Because the vast majority of testicular tumors are malignant there is a high chance the testis would have been removed anyway. Also, biopsying a malignant testicular tumor could allow tumor cells to seed in the scrotum.
CT of the thorax, abdomen, and pelvis should be made to look for spread, either before or after orchidectomy, but preferably before. This is necessary for staging. MRi of the brain is indicated if brain metastases are suspected.
Tumour markers
AFP, hCG, and LDH are important tumor markers in testicular tumors. Different histological subtypes have different patterns of expression of these tumor markers. Seminomas often do not have elevated tumour markers.
Hormone analysis
Before orchidectomy, we also measure hormone levels.
Stages
Limited disease refers to cancer which is limited to the testicles. Locally advanced disease is when there is involvement of the retroperitoneal lymph nodes, usually the para-aortic lymph nodes. Metastatic disease is when there is evidence of metastasis.
Management
All patients with suspected testicular cancer on ultrasound and physical examination should undergo surgical exploration. If surgery and intraoperative frozen histology sections cannot rule out malignancy, orchidectomy is performed. This allows for histological examination and complete staging and risk stratification. However, at no point should the urologic surgeon incise the tumour itself, for risk of seeding. A testicular prosthesis can be placed at the same time. If there is sign of retroperitoneal lymph node involvement, retroperitoneal lymph node dissection (RPLND) is indicated.
Localised disease with no high-risk features can usually be followed with active surveillance, but if there is intermediate or high-risk, adjuvant chemotherapy is recommended. In locally advanced disease, adjuvant radiotherapy or chemotherapy is indicated. For metastatic disease, adjuvant chemotherapy is indicated.
Organ sparing surgery
Organ sparing surgery, i.e. the resection of a tumour instead of complete orchidectomy, may be an option if the cancer affects both testicles or the patient only has one testicle and it is affected. The goal is to maintain the endocrine function of the testicles. Adjuvant radiotherapy is always indicated.
Biopsy of contralateral testicle
During orchidectomy, we may perform a biopsy of the contralateral (healthy-looking) testicle. This is to look for GCNIS (cancer in situ). This biopsy is indicated if the cancer is a germ cell tumour or there are risk factors of GCNIS, such as cryptorchidism or an atrophic testicle.
Chemotherapy
Chemotherapy is indicated if there is metastatic disease. It's usually a combination of cisplatin, etoposide, and bleomycin.
Radiotherapy
Seminomas are very radiosensitive, whereas non-seminomas are only moderately radiosensitive. For this reason, radiotherapy is mostly only used for seminomas. Radiotherapy is less and less used nowadays in favour of chemotherapy.
