17. Cancer of the pancreas and the liver
Pancreatic cancer
Pancreatic cancer, of which pancreatic adenocarcinoma is the most common histological type, is a malignancy with one of the highest mortality rates. It’s aggressive, causes no early symptoms, and is difficult to treat. It mostly affects elderly men.
Pancreatic cancer is the 10th most common cancer, but the fourth leading cause of cancer mortality. About 85% of cases are irresectable at the time of diagnosis due to being metastatic or locally advanced. It responds poorly to chemotherapy and grows quickly. The overall 5-year survival for all patients (regardless of stage) is < 5%, and even in the early stages the median survival is 2 years.
Etiology
Pathology
Pancreatic adenocarcinoma accounts for almost all malignant exocrine pancreatic cancer (the remaining being acinar adenocarcinoma and mucinous cystadenocarcinoma). Adenocarcinomas originate from epithelial cells of the pancreatic tubules.
60% of cases are located in the head of the pancreas, with the remaining 40% being spread evenly throughout the body and tail.
Stages
- Resectable disease
- 15% present in this stage
- Median survival of 20 – 24 months
- Locally advanced (unresectable) disease
- 25% present in this stage
- Median survival of 8 – 12 months
- Metastatic disease
- 50% present in this stage
- Median survival of 6 – 12 months
Clinical features
Pancreatic cancer generally causes no symptoms in the early stage, which contributes to the late diagnosis. Tumours in the pancreatic head cause symptoms earlier than tumours in the body or tail.
When symptoms do occur, jaundice, weight loss, anorexia, abdominal pain, vomiting, and constitutional symptoms may occur. Delayed gastric emptying occurs in up to 60% of people with pancreatic cancer and may contribute to the symptoms of anorexia and vomiting. Obstruction of the biliary tract is what leads to jaundice.
Invasion of nearby structures can cause chronic severe abdominal pain, usually belt-like and located to the epigastrium.
Courvoisier sign may be present. It refers to an enlarged, nontender gallbladder with painless jaundice. This contrasts with cholelithiasis, in which the gallbladder is tender.
Trousseau syndrome may also be present. It refers to a migratory, superficial thrombophlebitis.
Diagnosis and evaluation
Abdominal ultrasound is often the first investigation used in patients presenting with jaundice or epigastric pain. US is highly sensitive for pancreatic masses, and will show an echopoor lesion.
Contrast CT or MRI is required for proper staging and to determine whether it’s resectable or not. Pancreatic cancer is hypodense on CT. It will also show any distant metastases. CT of the thoracic cavity is also indicated to look for metastases.The tumour marker CA 19-9 may be elevated; if it is, it may be used for follow-up. Liver enzymes may be elevated if cholestasis has occurred.
The diagnosis requires histological confirmation, which is acquired by biopsy in most cases. However, if the suspicion is high and the mass appears to be resectable, the patient may skip biopsy and proceeds directly to surgery, where the diagnosis is made by intraoperative frozen sections.
Treatment
Even with curative treatment, the survival rate of pancreatic cancer is poor. Few patients have resectable disease at the time of diagnosis. Surgery is the only potentially curative treatment.
Curative modalities
There are two options for surgical treatment of pancreatic head tumours, conventional pancreaticoduodenctomy (Whipple procedure), and pylorus-preserving pancreaticoduodenectomy. Both should be combined with regional lymphadenectomy.
For resectable tumours in the body or tail of the pancreas, an extended distal pancreatectomy is performed, usually with splenectomy.
If the tumour is borderline resectable, neoadjuvant chemotherapy may be used in an attempt to achieve resectability. Adjuvant chemotherapy is frequently used, usually with gemcitabine or 5-FU, combined with erlotinib. Radiotherapy is not frequently used.
Palliative surgery for pancreatic and periampullary tumours
Many cases of pancreatic and periampullary cancer are irresectable and therefore incurable. Palliative surgery is therefore common.
Palliative surgery may be indicated for jaundice or gastric outlet obstruction in people with irresectable pancreatic cancer. These are usually managed with the placement of stents into the obstructed biliary tree or obstructed duodenum with ERCP. In case stent placement is impossible or insufficient, a bypass operation may be necessary.
Non-surgical palliative treatment
Pancreatic cancer pain usually requires opioid analgesics. Because the tumour may be close to the coeliac plexus, drugs effective against neuropathic pain may be used as adjuvants.
A permanent coeliac ganglion block (coeliac plexus neurolysis) can be used for pain management in case pharmacological therapy is insufficient. This involves radiographically guided puncture of the coeliac ganglion, followed by installation of ethanol, which destroys the nerve tissue permanently. Injection of a local anaesthetic instead produces temporary pain relief (and is mostly used for chronic pancreatitis).
Chemotherapy (with gemcitabine and erlotinib) may also be used for palliative therapy.
Liver cancer
Hepatocellular carcinoma (HCC) is the most common histological type of liver cancer. It’s mostly a disease of older men. In almost all cases it develops in an already cirrhotic liver, so the risk factors for HCC are the same as those for cirrhosis.
The incidence of HCC is increasing. Due to the long asymptomatic period, most cases are irresectable at presentation. This gives it a poor prognosis, with a 5-year survival of 30 – 50%.
Etiology
80% of HCC are preceded by cirrhosis, so the risk factors for HCC are similar to those of cirrhosis. However, some risk factors which are independent of cirrhosis are known:
Common causes:
- Chronic HBV or HCV infection
- Metabolic associated fatty liver disease
- Alcoholic liver disease
- Aflatoxin (rare outside the developing world)
Rare causes:
- Overuse of hepatotoxic drugs like paracetamol
- Haemochromatosis
- Autoimmune hepatitis
- Alpha-1-antitrypsin deficiency
- Wilson disease
- Hepatic adenoma
Pathology
HCC develops from a dysplastic nodule in a cirrhotic liver. This nodule is a precancerous lesion that can be visualized on ultrasound.
Hepatitis B may incorporate the HBsAg into the host genome. Hepatitis C has no such capacity. Both viruses increase cancer risk due to the chronic inflammation and high cell turnover they cause.
Aflatoxin causes a very characteristic mutation in the p53 gene called a signature mutation. If this mutation is present in an HCC it’s certain that the etiology was aflatoxin.
A special form of HCC called fibrolamellar HCC is very rare. Only 200 new cases are diagnosed every year. This type of HCC develops in young adults without cirrhosis or other risk factors for HCC.
Clinical features
The tumour itself is usually asymptomatic, but the patient usually has symptoms from the underlying disease (cirrhosis or hepatitis), like ascites and jaundice. Constitutional cancer symptoms like weight loss, weakness, abdominal pain may be present but may also be caused by the underlying disease.
Diagnosis and evaluation
Patients at high risk for HCC (cirrhosis of any cause, chronic hep B) should be screened regularly for HCC. Screening involves measuring abdominal ultrasound and AFP levels. Focal lesions in a cirrhotic liver are primary liver cancer until proven otherwise. AFP is elevated only in 50% of cases, in which case the level correlates with the tumour size.
Contrast CT or MR confirms the diagnosis and shows any extrahepatic spread. Typical features on imaging include early contrast uptake, “washout”, and vascular spread.
Liver biopsy is often not needed as the definitive diagnosis can be made with imaging, and biopsy carries a risk of bleeding and tumour spread.
Staging
The Barcelona Clinic Liver Cancer (BCLC) staging is the most frequently used staging system, and at least the one preferred in POTE. The Child-Pugh score and ECOG are important in determining the BCLC stage.
The Child-Pugh score involves multiple parameters that reflect liver function (bilirubin, albumin, PTT, INR, etc.) and classifies the function as Child-Pugh A, B, or C, where A is good liver function and C is poor liver function.
The BCLC staging determines which stage the disease is in, based on the TNM staging, ECOG, and Child-Pugh score:
- Very early stage (stage 0)
- Early stage (stage A)
- Intermediate stage (stage B)
- Advanced stage (stage C)
- Terminal stage (stage D)
Notably, a Child-Pugh C is BCLC terminal stage regardless of the TNM and ECOG features.
The so-called Milan criteria are used to evaluate whether the patient is a candidate for liver transplant or not. The Milan criteria are fulfilled if there is either a single tumour not > 5 cm, or up to 3 tumours, none of which are > 3 cm. There must also be no vascular invasion or extrahepatic spread.
Treatment
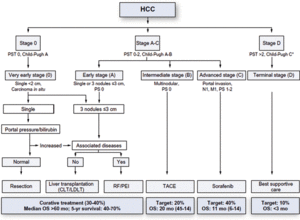
Generally, only BCLC stages 0 and A are curable. Curative modalities include surgical resection, liver transplantation, as well as local ablative techniques. The choice of modality depends on the BCLC stage. For terminal stage (D), no tumor-directed therapy is indicated; only palliative care is used.
Surgery
Surgical resection, preferably laparoscopically, is an option for very early or early stage liver cancer. Anatomical resection refers to resection which respects segmental and lobar anatomy. This may include segmentectomy (or bisegmentectomy or trisegmentectomy), hemihepatectomy, or sectionectomy. Atypical resection refers to resection which does not respect the liver anatomy.
Liver transplantation
Liver transplantation is a treatment option for early stage tumour. Liver transplantation is only considered if the Milan criteria are fulfilled.
Local ablation
Local ablation of the tumour, by radiofrequency or microwave ablation, or percutaneous ethanol injection, may be curative options in intermediate stage tumours.
TACE
Transarterial chemo-embolisation (TACE) is a minimally invasive technique which is the standard of care for patients with intermediate stage HCC. It involves intra-arterial injection of an emulsion of oil and a chemotherapeutic drug followed by embolisation of the blood vessel. The theory is that the combination of the chemotherapeutic drug and the ischaemia kills the cancer cells. TACE can not be used for cure and is therefore used with palliative intent.
Sorafenib
Sorafenib is a small molecule protein kinase inhibitor which is indicated for advanced stage HCC. It inhibits a variety of protein kinases. Sorafenib may be used as palliation in advanced stage HCC.
