Acute coronary syndrome: Difference between revisions
(Created page with "'''Acute coronary syndrome''' (<abbr>ACS</abbr>) is an umbrella term for acute presentations of coronary artery disease or ischaemic heart disease. ACS is used as an initial working diagnosis until an ECG and troponin level has been performed, which will decide which type of ACS the patient has. There are three types, each of which with differing underlying pathophysiology: * Non-ST elevation coronary syndrome (NSTE-ACS) ** Unstable...") |
No edit summary |
||
| Line 8: | Line 8: | ||
* [[ST-elevation myocardial infarction|ST elevation myocardial infarction]] (STEMI) | * [[ST-elevation myocardial infarction|ST elevation myocardial infarction]] (STEMI) | ||
STEMI and NSTEMI are both types of | STEMI and NSTEMI are both types of [[acute myocardial infarction]] (AMI). | ||
== Initial evaluation == | == Initial evaluation == | ||
| Line 31: | Line 31: | ||
All patients with suspicion for ACS should have their heart rhythm continuously monitored with a rhythm monitor. The risk for fatal arrhythmias is highest in the first days after an AMI. | All patients with suspicion for ACS should have their heart rhythm continuously monitored with a rhythm monitor. The risk for fatal arrhythmias is highest in the first days after an AMI. | ||
[[Category:Cardiology]] | [[Category:Cardiology]] | ||
<references /> | |||
[[Category:Internal Medicine (POTE course)]] | |||
Revision as of 10:21, 23 November 2023
Acute coronary syndrome (ACS) is an umbrella term for acute presentations of coronary artery disease or ischaemic heart disease. ACS is used as an initial working diagnosis until an ECG and troponin level has been performed, which will decide which type of ACS the patient has.
There are three types, each of which with differing underlying pathophysiology:
- Non-ST elevation coronary syndrome (NSTE-ACS)
- Unstable angina (UA)/unstable angina pectoris (UAP)
- Non-ST elevation myocardial infarction (NSTEMI)
- ST elevation myocardial infarction (STEMI)
STEMI and NSTEMI are both types of acute myocardial infarction (AMI).
Initial evaluation
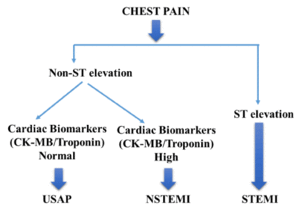
All patients presenting with sudden onset coronary chest pain or dyspnoea should take an ECG and a blood test to look for troponin levels. STEMI needs acute, urgent management, while NSTE-ACS needs a risk stratification before deciding the timing of management. High risk patients with NSTE-ACS should be treated acutely like STEMI, while low risk patients can be treated on a longer timescale. For this reason, it’s important to determine the type of ACS early, and if it’s either of the NSTE-ACS’s, perform a risk stratification.
The results from the ECG and troponin test will reveal the diagnosis:
- ST-elevations are present in ECG leads corresponding to a part of the heart supplied by a specific vessel -> the diagnosis is STEMI
- ST-elevations are not present in ECG leads corresponding to one part of the heart -> the diagnosis is NSTE-ACS
- Troponins are elevated and are dynamic -> the diagnosis is NSTEMI
- Troponins are not elevated -> the diagnosis is UA
In both STEMI and NSTEMI, the troponin levels increase, peak, and then start to decrease. For this reason, if you measure the troponin level at 2 different times in an AMI, the troponin level is going to be higher or lower at the second measurement, depending on whether the troponin peak had been reached or not at the time of the first measurement. This is called a rise and/or fall in troponin and is often referred to as troponin dynamics. Many conditions can cause troponin elevation, but troponin dynamics are highly specific for AMI. As such, if the diagnosis of AMI is not immediately certain, a repeat troponin measurement should be taken after 1 – 3 hours, and if a rise and/or fall is present, the diagnosis is certain. A significant rise and/or fall is defined as a change of > 20 – 50%.
However, the magnitude of troponin elevation corresponds to the myocardial damage. While conditions like heart failure and myocarditis also can cause troponin elevation, they virtually never cause a very large elevation in troponins. if the troponin levels are very high (even if only measured once), the risk for AMI is sufficiently high that we proceed to invasive management without waiting for a repeat troponin. Modern high-sensitivity troponin assays have an upper normal limit of normal of approx. 14 ng/L. As the single-measurement troponin increases beyond 1000 ng/L the specificity for AMI increases.
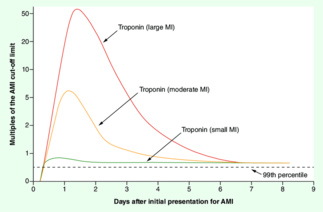
Modern high-sensitivity troponin assays can detect a rise in troponins 1 – 3 hours after the infarction. As such, the troponins may be normal if measured early. In these cases, a repeat measurement should be performed 1 – 3 hours later.
An echocardiography should also be performed in the emergency department. Regional hypokinesis or akinesis in regions corresponding to the blood supply territory of one coronary artery increases the likelihood that there is AMI. In addition, echocardiography may reveal alternative diagnoses, like aortic dissection, pericardial effusion, aortic stenosis, hypertrophic cardiomyopathy, or right ventricular dilation suggestive of acute PE.
All patients with suspicion for ACS should have their heart rhythm continuously monitored with a rhythm monitor. The risk for fatal arrhythmias is highest in the first days after an AMI.
